
Salt tablets. Compression stockings. A beta blocker that takes the edge off the tachycardia but doesn't touch the brain fog. Monthly cardiology appointments that go nowhere. Years of this. At some point, POTS stops being something anyone is trying to fix and becomes something you learn to work around.
Intensive programs promise a different deal: concentrated treatment over days or weeks instead of that slow drip of office visits spread across years. The word "intensive" sounds good. But it means wildly different things depending on who's offering it. Some programs are just the same standard care compressed into a shorter calendar — the stuff that wasn't working, delivered faster. Others are built on a fundamentally different model of what POTS actually is.
This guide is about telling those apart.
What Makes a Program "Intensive"?
In clinical terms: concentrated treatment over consecutive days, multiple hours per day, instead of weekly or biweekly visits stretched over months. The duration varies by patient and complexity — there's no fixed number that applies to everyone.
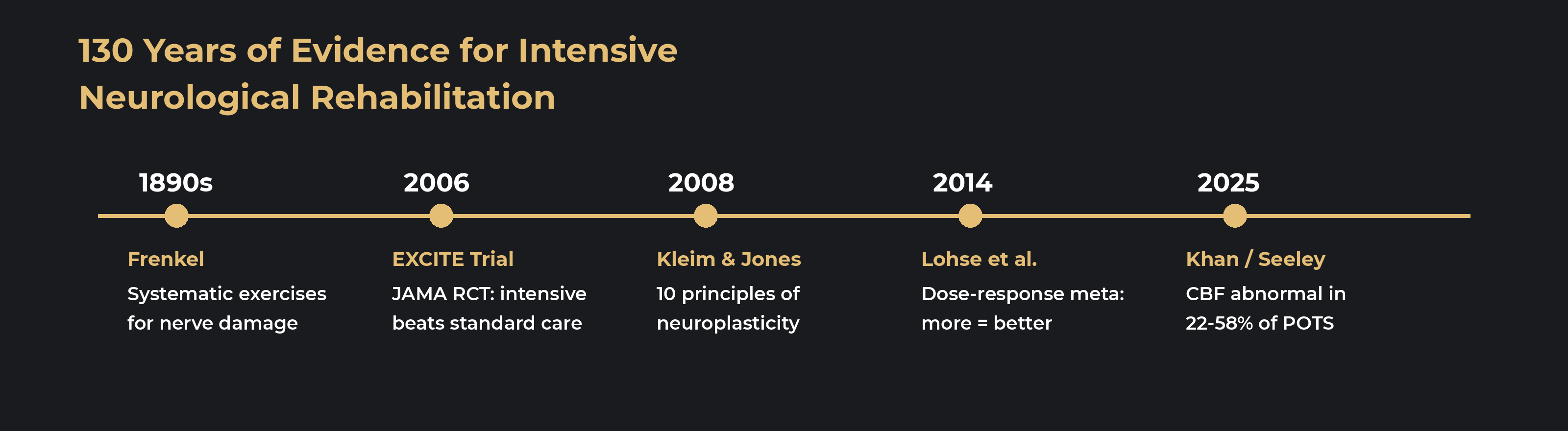
The idea isn't new. In the 1890s, a Swiss neurologist named Heinrich Frenkel developed a system of intensive, repetitive exercises for patients with tabes dorsalis — syphilitic degeneration of the spinal cord that destroyed proprioceptive function. His patients had documented structural nerve damage. Conventional wisdom said they couldn't improve. Frenkel proved otherwise through graded, concentrated, daily practice that substituted visual feedback for lost proprioception (Zwecker et al., Spinal Cord, 2004). That was 130 years ago, and the principle hasn't changed: the nervous system reorganizes through intensity, repetition, and specificity — not through occasional visits.
Modern neuroscience explains why. Kleim and Jones identified ten principles of experience-dependent neural plasticity, including that sufficient intensity is required to drive adaptation — subthreshold stimulation simply doesn't produce plastic change (Kleim & Jones, JSLHR, 2008). Lohse and colleagues confirmed the dose-response relationship in a meta-analysis: more therapy time produces measurably better outcomes, with effect sizes increasing as scheduled therapy time increases (Lohse et al., Stroke, 2014).
The landmark proof came from the EXCITE trial. Wolf and colleagues randomized 222 stroke patients to either intensive constraint-induced movement therapy — 6 hours per day for 2 weeks — or usual care. The intensive group showed significantly greater functional improvement, with benefits persisting at 12-month follow-up (Wolf et al., JAMA, 2006). Subsequent research by Taub showed that this wasn't just functional improvement — intensive practice produced measurable cortical reorganization visible on fMRI and TMS (Taub et al., Frontiers in Human Neuroscience, 2014).
The same principle applies to autonomic rehabilitation directly. Ector and colleagues demonstrated that daily in-hospital tilt training — intensive, repeated orthostatic exposure at 60 degrees — eliminated syncope in 13 of 13 patients with refractory neurocardiogenic syncope. Home maintenance with standing exercises sustained the results (Ector et al., PACE, 1998). Weekly visits wouldn't have produced the same retraining of the autonomic reflex arc. Daily exposure did.
POTS involves dysregulated autonomic circuits. Immersive treatment creates conditions for those circuits to actually reorganize. The brainstem doesn't learn new regulatory patterns from an exercise you did last Tuesday. It learns from sustained, calibrated input that builds on itself hour by hour, day by day.
But the format only matters if the treatment is targeting the right thing.
The Four Approaches to Intensive POTS Treatment
Four broad categories. They differ in what they test, what they treat, how long they take, and what evidence supports them. The word "intensive" doesn't tell you whether the approach matches your specific mechanism.
| Medication Management | Cardiac Rehab / Exercise | Biofeedback / ANS Retraining | Brain-First / Mechanism-Based | |
|---|---|---|---|---|
| What they test | HR, BP, tilt table, sometimes catecholamines | HR, BP, exercise capacity (VO2 max) | HRV, skin conductance, sometimes respiratory rate | CBF (TCD), CO2 (capnography), VNG, vestibular function, cognitive testing |
| What they treat | Heart rate, blood pressure, blood volume | Cardiovascular deconditioning, exercise tolerance | Autonomic tone, stress response, breathing patterns | Specific regulatory failure: CBF dysregulation, vestibular error, proprioceptive input, brainstem coordination |
| Typical duration | Ongoing (not time-limited) | 3–6 months outpatient; 2–4 weeks intensive | 6–12 weeks; sometimes 1–2 week intensive | Variable (consecutive days), follow-up protocol |
| Outcome measure | Symptom reduction, HR control | Exercise capacity, orthostatic tolerance | HRV improvement, subjective symptom reduction | Pre/post CBF velocity, CO2 normalization, functional improvement |
| Evidence basis | RCTs for individual drugs (propranolol, ivabradine, midodrine) | Levine protocol RCTs; CHOP protocol observational | Small studies, mostly uncontrolled | CBF research (JAHA 2025, Novak 2024); vestibular-autonomic literature; clinical outcomes |
| Key limitation | Doesn't address mechanism; manages outputs | Assumes deconditioning is the cause | Treats the output without identifying the input error | Fewer large RCTs; requires specialized diagnostic equipment |
Medications keep some people functional enough to participate in rehabilitation. Exercise improves cardiovascular fitness. Biofeedback can reduce symptom perception. None of those are "wrong." The question is whether any of them match the mechanism driving your symptoms.
Medication Management
Medication isn't "intensive" in the concentrated-treatment sense, but it's where most POTS patients start, so it's worth being honest about what it does and doesn't do.
Beta blockers (propranolol, metoprolol), ivabradine, midodrine, fludrocortisone — each targets a specific physiological parameter. Propranolol slows the heart rate. Midodrine raises blood pressure. Fludrocortisone expands blood volume. The evidence for individual drugs is real. Raj and colleagues showed in 2009 that low-dose propranolol (20mg) outperformed high-dose (80mg) for POTS, because the low dose reduced heart rate without tanking stroke volume (Raj et al., Circulation, 2009).
But every one of these drugs manages an output. The heart rate was elevated for a reason. The blood pressure was low for a reason. Block the output, and you may get symptom relief — but the upstream mechanism is still running.
For patients whose primary driver is cerebral blood flow dysregulation, medications that focus on peripheral cardiovascular parameters miss the point entirely. That's managing the dashboard without looking under the hood. Some patients do need pharmacological support as a bridge — especially when symptoms are severe enough to prevent participation in rehabilitation. But medication as the entire treatment plan is a ceiling, not a solution.
Cardiac Rehabilitation and Exercise Programs
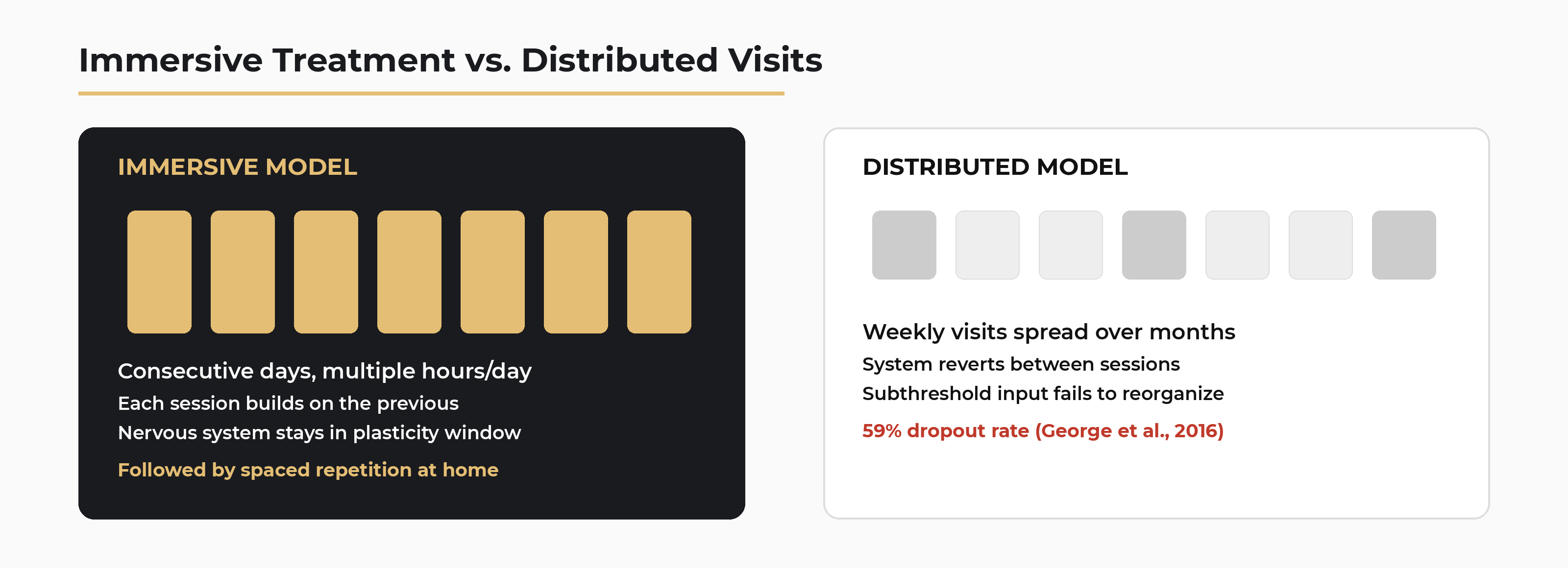
59% of POTS patients couldn't complete the Levine protocol.
That number, from George and colleagues (George et al., Heart Rhythm, 2016), tells you a lot about the gap between what exercise programs ask of POTS patients and what POTS patients can actually do. The Levine protocol (UT Southwestern) and CHOP protocol (Children's Hospital of Philadelphia) both use structured, progressive exercise over 3 to 6 months. Levine starts with recumbent exercises and gradually moves upright.
Exercise helps. Multiple studies show improvements in orthostatic tolerance, stroke volume, and quality of life. That's not in question.
What is in question is the assumption underneath: that deconditioning is the primary driver. For some patients it is, and they respond well. But research over the past decade keeps showing that deconditioning is often a consequence of POTS, not its cause. If the reason you can't exercise is that your brain isn't getting adequate blood flow when you're upright, cardiovascular conditioning won't fix the blood flow regulation problem. You're strengthening the engine while the fuel line is kinked.
Biofeedback and ANS Retraining
HRV biofeedback, paced breathing protocols, meditation-based autonomic retraining — these target the autonomic nervous system's output patterns, training patients to increase heart rate variability or shift autonomic balance. Some run as intensive retreats over 1 to 2 weeks. There's modest evidence for symptom reduction.
The conceptual problem: biofeedback measures an output (heart rate variability, skin conductance) and tries to change that output through volitional effort. If the dysregulation originates in the brainstem's central coordination — in how it integrates vestibular, proprioceptive, and respiratory inputs to organize autonomic output — training someone to alter a downstream readout doesn't touch why the readout was abnormal. You're adjusting the display without fixing the circuitry.
Brain-First, Mechanism-Based Intensive Rehabilitation
Different starting question. Not "how do we control the heart rate?" or "how do we improve exercise tolerance?" but: "Why is the autonomic system dysregulated, and where in the regulatory chain is the failure?"
Answering that requires different diagnostic tools. Transcranial Doppler ultrasound to measure cerebral blood flow in real time. Capnography to track CO2 dynamics. Videonystagmography (VNG) to assess vestibular function. Comprehensive neurological examination to identify which brainstem circuits, cerebellar pathways, or proprioceptive inputs are contributing to the dysregulation. Once the mechanism is identified — CBF regulation failure? Vestibular coordination error? Corrupted cervical proprioception? Impaired respiratory integration? — treatment is built around that specific finding. Not a generic protocol applied to everyone with a POTS diagnosis.
The Two-Phase Model: Immersion Then Spaced Repetition
An intensive isn't a cure compressed into a week. It's the first phase of a two-phase process.
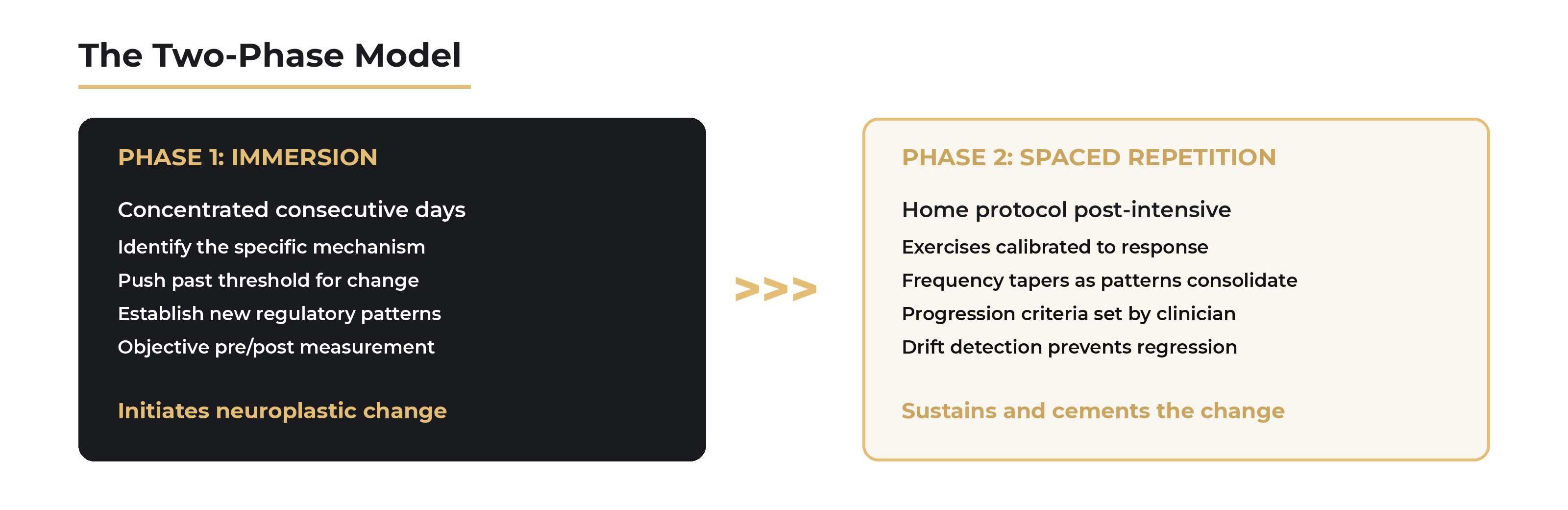
Phase 1: Immersion. Dense, concentrated input over consecutive days. This is where you identify the mechanism, push the nervous system past its threshold for change, and establish new regulatory patterns. The brainstem needs sustained, calibrated input — multiple sessions per day, each building on the last — to begin reorganizing circuits that have been running the wrong program for months or years. A weekly visit can't generate the same momentum. The system reverts between sessions. Immersion keeps it in the window of plasticity long enough for actual reorganization to begin.
Phase 2: Spaced repetition. The intensive ends. The work doesn't. What you take home is a specific protocol — exercises calibrated to what responded during the intensive, performed on a prescribed schedule that your clinician designs based on how your nervous system responded. Frequency starts high and tapers as the patterns consolidate. The immersive phase initiated the change. Spaced repetition cements it into the system's default operating state.
This is the same learning model behind skill acquisition in every domain. Intensive practice creates the initial adaptation. Spaced repetition prevents regression and converts temporary change into durable reorganization. Without the intensive, the change never gets started. Without the spaced repetition, it doesn't stick.
Any program that gives you an intensive and no follow-up protocol is doing half the job. Any program that gives you only weekly visits for months is trying to get neuroplastic change from subthreshold input. The two phases aren't interchangeable. You need both, in that order.
Why the Mechanism Matters for Choosing a Program
The intensive format is the right delivery system. But it only works if it's delivering the right treatment. Recent research has clarified what's actually driving POTS symptoms in a substantial proportion of patients — and it changes which treatment approach makes sense.
Khan and colleagues' systematic review found that 22–58% of POTS patients have measurably abnormal cerebral blood flow during tilt testing (Khan et al., JAHA, 2025). Novak's group showed that POTS and hypocapnic cerebral hypoperfusion are the same disorder on a spectrum (Novak et al., Frontiers in Neurology, 2024). The tachycardia isn't the disease — it's a compensatory response to reduced brain blood flow. For a deeper look at this mechanism, see our articles on why heart rate isn't the problem and hypocapnic cerebral hypoperfusion.
If your primary driver is cerebral blood flow dysregulation, an intensive cardiac rehab program won't reach the problem. Exercise improves cardiovascular fitness — genuinely — but it doesn't fix why the brain's blood flow regulation is failing. You need an intensive that targets the specific upstream error: vestibular input, cervical proprioception, brainstem coordination, respiratory integration. And you need to know which of those is broken before treatment starts.
How to Evaluate Any Intensive Program
Whether you're looking at our clinic or anyone else's, six questions separate programs built on mechanism identification from programs running protocols.
- Do they measure cerebral blood flow, or just heart rate and blood pressure? Standard tilt testing that only monitors peripheral vitals cannot detect the CBF abnormalities present in 22–58% of POTS patients. Transcranial Doppler during orthostatic challenge is the minimum required to assess brain perfusion. If a program doesn't include this, it cannot identify or track the most common measurable abnormality in the condition it claims to treat.
- Do they identify a specific mechanism before starting treatment? "You have POTS" is a syndrome label, not a mechanism. The mechanism might be impaired cerebral autoregulation, hypocapnia-driven vasoconstriction, vestibular-autonomic dysfunction, cervical proprioceptive error, or some combination. Each requires a different intervention. A program that starts everyone on the same protocol regardless of mechanism is guessing.
- Do they re-measure after treatment to verify improvement? Pre/post objective data is the difference between "you feel better" and "your brain blood flow velocity improved from 38 cm/s to 52 cm/s on tilt." Feelings are valid. Measurements are verifiable. A serious program provides both.
- What diagnostic technology do they actually use? Transcranial Doppler, VNG, capnography, and comprehensive neurological examination can identify mechanisms. HRV biofeedback alone measures an output without identifying why the output is abnormal. The diagnostic tools determine the diagnostic precision.
- What is the treatment-to-assessment ratio? If you spend three days on testing and two days on treatment, ask why. Conversely, if you get zero objective assessment and jump straight into a protocol, ask what the protocol is based on. A well-designed intensive program front-loads assessment, then adjusts treatment in real time based on what the assessment reveals.
- Do they provide a post-program protocol? Neuroplastic changes initiated during an intensive need to be maintained. The brainstem doesn't finish reorganizing during the intensive — it creates the conditions for change and gets the process moving. A post-program protocol with specific exercises, frequencies, and progression milestones is what sustains those gains. Ask what happens after you leave.
What a Brain-First Intensive Actually Looks Like
In our clinic, the structure follows the mechanism, not a template. But here's the general framework.
Assessment phase. Transcranial Doppler on tilt — measuring cerebral blood flow velocity in the middle cerebral arteries while transitioning from supine to upright. Capnography tracking end-tidal CO2 throughout. VNG to map vestibular function in detail. Oculomotor testing. Cervical proprioceptive assessment. Cognitive testing under orthostatic challenge. The goal isn't to confirm you have POTS — you already know that. The goal is to identify where in the regulatory chain your system is failing and how badly.
Treatment phase. Calibrated to the specific regulatory failures identified in assessment. The exact combination and intensity changes patient to patient — and sometimes day to day within the same patient as the system responds. Common modalities include:
- Vestibular rehabilitation — recalibrating the sensory inputs the brainstem relies on when coordinating blood pressure and blood flow regulation during position changes. The vestibulo-sympathetic reflex is a direct pathway from the inner ear to autonomic cardiovascular control (Yates, 2000). Corrupted vestibular input means corrupted autonomic regulation.
- Oculomotor exercises — specific eye movement patterns that drive brainstem circuits directly involved in autonomic control. Not generic "eye exercises." Selected based on which brainstem pathways showed dysfunction during assessment.
- Cervical proprioceptive work — the neck sends critical position data to the brainstem. Bolton and colleagues demonstrated that cervical afferent input directly modulates cardiovascular autonomic function (Bolton et al., 2014). If that signal is corrupted — from prior injury, poor motor control, structural changes — autonomic and vascular regulation both suffer. We clean up the input.
- Respiratory integration — and this is a crucial distinction. We don't coach you to breathe differently on purpose. We target central integration so your breathing naturally recalibrates to match metabolic demand, producing stable CO2 levels without conscious effort. Volitional breathing retraining asks you to consciously control something that should be automatic. Central respiratory recalibration restores the automatic process itself. The difference in outcome is significant.
- Graded tilt oscillation — progressive postural challenges that retrain the baroreceptor and cerebrovascular reflexes. Start at the angle and duration the patient can tolerate. Incrementally progress. Track CBF with TCD during the process — if blood flow drops below threshold, we modify. If it holds, we advance. Precision, not protocol.
Re-assessment and post-program design. Same objective measurements as the initial assessment. Compare the numbers. Where did CBF velocity improve? Where did CO2 stabilize? What vestibular findings changed? Then build a home protocol — specific exercises, frequencies, progression milestones — based on what responded and what still needs work.
We track it all objectively. Transcranial Doppler and capnography before, during, and after treatment sessions. When a patient's CBF velocity on tilt goes from a 35% drop to a 12% drop over the course of treatment, that's not a placebo effect. That's a measurable change in how the brain is regulating its own blood supply.
Why Concentration Matters (and Why Weekly Visits Often Stall)
Neuroplasticity has rules. Kleim and Jones mapped ten of them. The one that matters most here: sufficient intensity is required to drive neural adaptation. Below a threshold of repetition and sustained input, the nervous system simply doesn't reorganize (Kleim & Jones, 2008).
A session once a week allows the nervous system to return to its default state between visits. You push the system, it starts to shift, six days pass, it drifts back. Progress is glacial because you're fighting the system's tendency to revert between inputs.
The EXCITE trial demonstrated the alternative. Intensive constraint-induced movement therapy — 6 hours per day for 2 consecutive weeks — produced functional gains that persisted at 12 months. Usual-care therapy distributed over the same period did not produce the same results (Wolf et al., JAMA, 2006). Lohse and colleagues' meta-analysis quantified the relationship: the more therapy time scheduled, the larger the effect sizes, with the relationship holding across multiple rehabilitation domains (Lohse et al., Stroke, 2014).
For autonomic rehabilitation specifically, Ector demonstrated that daily tilt training eliminated syncope in all 13 patients tested — an outcome that occasional outpatient visits had failed to produce (Ector et al., PACE, 1998). The autonomic nervous system, like the motor system, responds to concentrated repetition. It doesn't reorganize from distributed, subthreshold exposure.
There's also the practical reality that many POTS patients travel from out of state or out of country for specialized care. Weekly visits for six months isn't an option when you're flying in from overseas. A concentrated intensive is often the only realistic path for this population.
What Happens After You Leave
This is where most intensive programs fall short. Treatment, a handshake, and "good luck." The neuroplastic changes initiated during the intensive are real but fragile. Without a structured post-program protocol, the nervous system drifts back toward its old patterns.
A well-designed post-program protocol includes specific exercises prescribed based on what responded during the intensive — not a generic sheet. Frequency and progression should be tailored by your clinician based on how your nervous system responded. There should be clear criteria: what needs to be true before you advance, and what to do if you hit a setback. And there should be a way to check in — objectively, not just "how do you feel?" — so drift gets caught before it costs you weeks of progress.
The intensive creates the conditions for change. The post-program protocol is what determines whether that change becomes permanent. Ask any program you're considering: what exactly do I take home, and how do I know if it's working?
What You Can Do Right Now
Before you book anything — a few steps that will help you evaluate your options, regardless of which direction you go.
1. Request your existing test results. If you've had a tilt table test, get the raw data — not just the summary letter. Look for whether cerebral blood flow was measured. In most cases, it wasn't. That gap tells you something about what could still be undiagnosed.
2. Use the six evaluation questions. Ask them when you talk to any program. You'll know within five minutes whether they identify mechanisms or apply protocols.
3. Track your own patterns. Keep a simple daily log: what time symptoms are worst, what positions trigger them, what makes them better or worse. Patterns that emerge over weeks often point directly to the regulatory failure. Morning-dominant symptoms suggest one mechanism. Post-meal crashes suggest another. Post-exertional malaise points to a third. This data is genuinely useful to any clinician trying to identify your specific mechanism.
4. Understand your current medications. Know what each one is doing and what it's blocking. If you're on a beta blocker, you're reducing a compensatory tachycardia. That may be necessary. But it means something upstream is still driving the need for that compensation, and that upstream driver needs to be identified. All medication decisions should be made with your prescribing physician.
5. Don't stop exercising. Exercise genuinely helps cardiovascular fitness in POTS, even when the primary mechanism is something else. Exercise alone can't fix a cerebral blood flow regulation problem — but both things are true simultaneously. Move as much as you can without crashing, and pursue mechanism identification in parallel.
6. Question "normal" test results. If you've been told your tilt test was normal but you can barely function, the testing may have been incomplete. A normal tilt test that only measured heart rate and blood pressure cannot rule out orthostatic cerebral hypoperfusion. It simply didn't look for it.
Key Takeaways
- Effective POTS rehabilitation has two phases: immersion then spaced repetition. The intensive initiates neuroplastic change. The home protocol sustains it. You need both.
- The evidence for intensive rehabilitation comes from 130 years of neurological practice — from Frenkel's exercises in the 1890s through the EXCITE trial (JAMA, 2006) and modern dose-response research (Lohse et al., Stroke, 2014).
- "Intensive" means different things depending on the program. Concentrated timing matters for neuroplasticity, but only if the treatment targets the right mechanism.
- A program worth evaluating should identify the specific mechanism before treatment starts, use objective measurement, provide pre/post data, and send you home with a structured protocol.
- Ask what happens after the intensive ends. If the answer is vague, the program is doing half the job.
Get the Free POTS Roadmap
The 4 mechanisms your doctors aren't testing for — and how to find which one is actually keeping you sick.
Download the RoadmapConsidering an Intensive Program?
A free discovery call with Dr. Keiser can help determine whether mechanism-based intensive rehabilitation fits your situation — and what testing should come first.
Schedule a Free Discovery CallDr. Keiser is a board-certified chiropractic neurologist (DC, DACNB, FABBIR), not a medical doctor (MD/DO). This content is for educational purposes and does not constitute medical advice. It is not a substitute for professional medical evaluation, diagnosis, or treatment. Always consult a qualified healthcare provider about your specific situation. Medication decisions should be made with your prescribing physician.