POTS Is a Description, Not an Explanation
Your POTS diagnosis told you what's happening. It didn't tell you why. Understanding the difference is the key to actually getting better.
Read Article

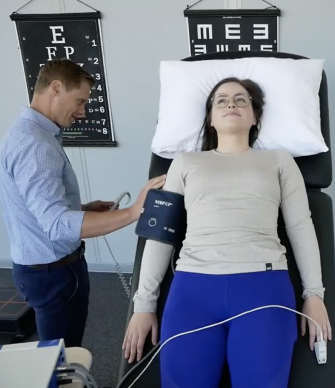
Why We Use Transcranial Doppler for POTS
Heart rate is only part of the story. Measuring actual blood flow to the brain reveals what's really happening when you stand up.

What Your Eye Movements Reveal About Your Brain
Eye tracking isn't just for research labs. It's one of the most powerful tools we have for assessing brain function.

When Rest Isn't Enough: Treating Persistent Post-Concussion Symptoms
The old advice was to rest until symptoms resolve. For many patients, that never happens. Here's what actually works.
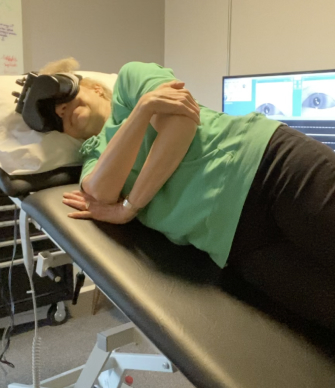
The 5 Types of Vestibular Dysfunction (And Why It Matters)
Not all dizziness is the same. Identifying which component of your vestibular system is affected determines what treatment will work.

Beyond the Tilt Table: Comprehensive Autonomic Testing
A positive tilt table test confirms POTS. But it doesn't tell you why. Here's what we test to find the actual mechanism.
Migraine as a Neurological Event: A Different Approach
Medication manages the pain. But migraine is more than pain — it's a neurological event. Treating it that way opens new options.
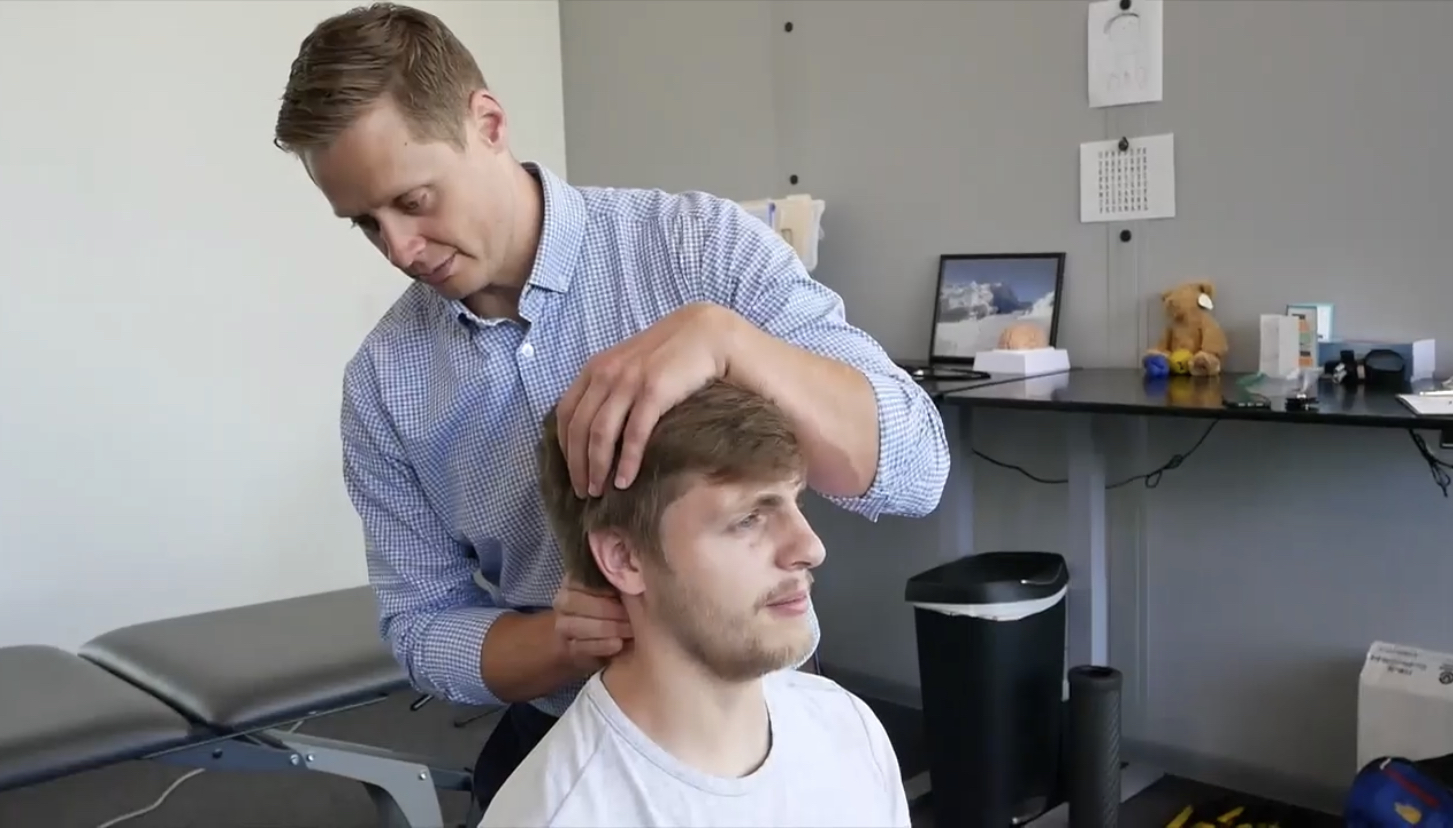
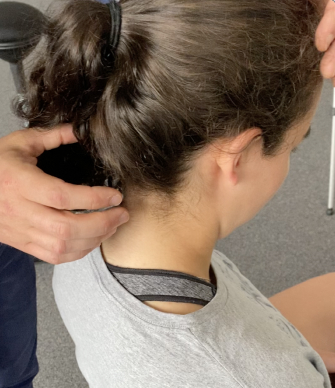
How Your Neck Affects Your Brain: 7 Ways Cervical Joint Errors Drive Symptoms
Your neck does far more than hold your head up. When cervical joints aren't working properly, the consequences reach your brain.

Is Small Fiber Neuropathy Causing Your Dysautonomia?
Neuropathy doesn't mean your nerves are dead. Understanding the type you have changes everything about treatment and prognosis.
Brain Fog Isn't a Diagnosis: What's Actually Happening in Your Brain
Brain fog is a symptom, not a condition. Treating it directly without understanding the mechanism is why so many people stay stuck.
Exercise Intolerance in POTS: It's Not Just Deconditioning
When "just exercise more" makes everything worse, the problem isn't effort. It's what the brain is doing with blood flow during exertion.

Can Posture and Spinal Alignment Actually Affect Blood Flow to Your Brain?
Structural issues CAN change cerebral perfusion — but only if that's actually the impediment to blood flow in the first place.

Is IV Saline the Cure for ME/CFS and Dysautonomia?
IV fluids make you feel better for a few hours. But if the problem isn't total volume, why would adding more volume be the answer?

How to Actually Diagnose Chronic Fatigue Syndrome
ME/CFS isn't just being tired. It's a real, measurable neurological condition — and diagnosing it properly starts with finding the mechanism.

How to Reverse PEM for Good (ME/CFS Recovery)
The crash has a mechanism. Understanding that mechanism is how you stop post-exertional malaise from running your life.

Functional Neurological Disorder (FND) and POTS
FND is one of the most misunderstood diagnoses in neurology. Here's what it actually means and why it's not "all in your head."

The Reason Your Brain Isn't Getting Enough Blood
Normal blood pressure doesn't mean normal brain blood flow. Here's why that gap exists and what it means for your symptoms.

Why Most Dysautonomia Treatments Don't Work
You've tried the medications, the salt, the compression stockings. If they're not working, the problem might not be the treatment — it might be the diagnosis.

Can Vitamin Toxicity Be Causing Your POTS?
Everyone talks about deficiency. Almost nobody talks about toxicity. But too much of certain supplements can make your autonomic symptoms worse.

POTS: When Your Brain Loses Its Balance
POTS isn't just a heart rate problem. It's what happens when your brain can't properly coordinate the systems that keep you upright.

Blood Pooling Is NOT Caused by "Loose Veins"
The "floppy veins" explanation is everywhere. But the actual mechanism is more interesting — and more treatable — than that.

The Root Cause of Tachycardia in POTS
Your heart rate spikes when you stand up. Everyone focuses on slowing it down. But the tachycardia isn't the problem — it's a symptom.

Is Deconditioning Causing Your POTS?
"Just exercise more" is the most common advice. But is deconditioning really the cause — or a consequence of something else going wrong?

Sleep, Neuroplasticity, and POTS: Why Your Brain Needs Sleep to Heal
Sleep isn't rest — it's a highly regulated, actively restorative process. If your brain is already struggling, it changes everything about how you recover.

Proof That the Brain Controls the Autonomic System
When we stimulate the brain in the right way, we can watch the autonomic outputs change — in real time, on every measure we track.

Case Study: POTS and Digestion Problems Solved Together
A 21-year-old with dysautonomia and gastroparesis improved digestion, heart rate, and sensation through neural rehabilitation — without any GI-specific treatment.

Case Study: 2 Years of POTS Resolved in One Month
How we used cerebral blood flow testing, tilt angle progression, and retinal slip exercises to rebuild orthostatic tolerance from the ground up.

EDS and POTS: Back to Life in Less Than a Month
A college-aged patient with Ehlers-Danlos Syndrome and POTS went from missing school and extreme fatigue to getting back on track.

POTS Treatment: From Housebound to Coaching Again
A 21-year-old college athlete couldn't drive, shop for groceries, or attend school. Here's how we approached his case — and what happened.

What a Tilt Test Really Reveals About POTS
A real case study walking through the tilt test data — what the blood flow numbers actually show and why one side dropped and the other didn't.

Hyperadrenergic POTS: When the Brakes Fail
Autonomic hyperactivity isn't just "too much adrenaline." It's what happens when the brain stops providing the inhibition that keeps the system in check.

Diagnosed With POTS — But That Wasn't the Problem
A 15-year-old with severe migraines, dizziness, and air hunger had been diagnosed and treated for POTS. The real issue was in the brain.

Solving Post-Concussion Symptoms That Wouldn't Go Away
Dizziness, heart rate spikes to 170, sweaty hands, nausea, and broken sleep. Here's how we found the problem in the eyes and rebuilt it step by step.

8-Year POTS Recovery: From Wheelchair to Walking in 3 Weeks
After 8 years of POTS and daily wheelchair use, a patient left the chair behind in just a few weeks through targeted brain rehabilitation.

How SSRIs Affect POTS Symptoms: What You Need to Know
Dr. Keiser explains how stimulant medications affect POTS symptoms, why your body compensates with energy mobilization, and how sunlight plays a role.

POTS or Anxiety? How to Tell the Difference
Loads of people with POTS are diagnosed with anxiety as a brush-off. Here's how we figure out which is actually driving the symptoms.

What Doctors Are Missing in POTS Cases
Why standard workups miss the real problem in POTS, and why clean MRIs and normal blood work don't mean nothing is wrong.

How to Know If Your POTS Is Actually Improving
Heart rate isn't the only measure of progress. Dr. Keiser explains what real POTS improvement looks like beyond the numbers.

Orthostatic Intolerance Explained: What It Is and Why It Happens
A complete breakdown of orthostatic intolerance — what causes it, how it differs from POTS, and why blood flow to the brain matters more than heart rate.

POTS Recovery After 2 Weeks of Treatment: A Case Study
Case study showing measurable POTS improvement after just two weeks of targeted neurological rehabilitation.

What Is Functional Neurology? How It Works and Who It Helps
Dr. Keiser explains what functional neurology actually is, how it differs from traditional neurology, and what kind of patients benefit most.

Your Brain's Secret Blood Flow Control System
Your brain controls its own blood supply separately from the rest of your body. When that system fails, standard treatments can't reach the problem.

Tilt Table Test for POTS: Everything You Need to Know
Getting a tilt table test? Dr. Keiser clears up the biggest misconceptions and explains what a good tilt test should actually measure.

Mast Cells and Your Autonomic System: The Connection Nobody Explains
Mast cell activation and POTS are connected through specific sympathetic pathways. How histamine drives blood pooling and autonomic compensation.

Recalibrate, Don't Just Manage
POTS treatment should recalibrate your nervous system, not just manage symptoms. Why targeting the lynchpin unlocks recovery.

Why Your Diagnosis Label Might Be Holding You Back
CFS, POTS, and ME/CFS syndrome labels describe symptoms, not causes. Moving from syndrome to mechanism is the key to effective treatment.

The Autonomic System Isn't a Switch (And Why That Matters)
Why "sympathetic dominance" is misleading and how specific autonomic pathways — not an on/off switch — drive POTS symptoms.

The "Little Brain" That May Be Causing Your Dysautonomia
The cerebellum regulates autonomic reflexes. When it's not calibrating properly, POTS and dysautonomia symptoms follow.

The Vagus Nerve Isn't What You Think
Vagus nerve stimulation for POTS misses the point. The vagus nerve is mostly sensory, and "paired antagonism" is a myth.

Why Standard Exercise Advice Fails POTS Patients
Exercise advice fails POTS patients because it ignores orthostatic blood flow. Fix cerebral perfusion first, then build capacity.

Why You Feel Better In The Car (And Worse When It Stops)
Mal de Debarquement Syndrome explains why passive motion feels better. The sensory mismatch driving your symptoms.

Why Your Heart Rate Isn't the Problem in POTS
POTS heart rate spikes are compensatory, not the root problem. Cerebral blood flow, not tachycardia, is the real issue.

Your Neck Might Be Part of the Problem
Neck stiffness with dysautonomia isn't random. The neurological connection between your cervical spine, vestibular system, and autonomic symptoms.

You're Not Lazy — Your Brain Is Running on Empty
POTS fatigue and brain fog aren't laziness. Reduced cerebral blood flow starves your brain of fuel. Here's what testing reveals.

What Happens When a Concussion Doesn't Heal
Post-concussion symptoms that persist involve disrupted cerebral blood flow and cerebellar dysfunction. The brain mechanisms behind lingering recovery.
